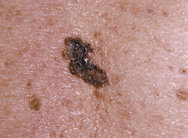
Melanoma
What is Melanoma?
Melanoma is a very serious type of skin cancer that can appear at any age. People with light skin, hair and eyes are at a higher risk, as are those who have a family history of the disease or have previously had melanoma themselves. Ultraviolet rays from sunlight or tanning beds are the key contributing environmental factor.Melanoma is less common than other types of skin cancer, accounting for only about 1-2% of all skin cancers, but extremely serious and more dangerous if not found early. Melanoma causes around 75% of skin-cancer-related deaths.When melanocytes, the cells responsible for skin color, grow out of control, the resulting tumors are called melanoma. It can form anywhere melanocytes are found on the body or spread to internal organs, making early detection critical. Melanomas may develop suddenly, but more often changes in an existing mole will alert you to the possibility of a skin cancer.
ABCDEs of Melanoma?
In order to help identify possible melanomas yourself, it is helpful to remember the “ABCDEs” for unusual moles

Asymmetrical Shape
Check moles for irregular shapes, particularly if one half of the growth does not match the other.
Border Irregularities
Moles with notches or jagged borders are characteristic of melanoma.
Color
Melanomas are black, brown, multicolored or unevenly colored.
Diameter
Be alert for any increase in size, especially moles over 1/4 inch.
Evolving
Any change in an existing mole, including in size, color, and shape, or moles that become itchy or bleed are cause for consulting your dermatologist.
Since exposure to the sun is a factor in so many cases of melanoma, one way to protect yourself is to limit your time in the sun, especially between 10 a.m. and 4 p.m. when the sun’s rays reach their peak. Always wear sunscreen with an SPF (Sun Protection Factor) of at least 30 with protection against both ultraviolet A (UVA) and ultraviolet B (UVB) rays and reapply it every couple of hours. Wear protective clothing and sunglasses and stay in the shade when possible. Avoid tanning beds and be careful around anything that can reflect the sun’s rays, such as water, sand, and snow.
What You Need to Know
-
Melanoma is a very serious cancer, but the prognosis is good when diagnosed and treated early
-
Avoid sun exposure and wear sunscreen to reduce your chances of getting melanoma
-
Checking your own skin once a month for abnormalities and changes can lead to early detection
-
Melanoma is diagnosed through a biopsy and your doctor will discuss treatment options with you
Check Yourself
You can also help protect yourself by examining your own skin once a month. It is often difficult to diagnose skin cancer just by appearance. This is why it’s so important for you to check your own skin and notify your doctor of anything you find. Examine yourself from head to toe, using a mirror when necessary. Look for any changes to existing moles and freckles, sores that take more than 3 weeks to heal, spots that hurt or itch continuously, growths that have increased in size or are larger than a pencil eraser, irregular outlines or changes in color or texture. If you note any changes in your skin, see your dermatologist. Know Your Spots >>
Diagnosis and Treatment
Your doctor will take a biopsy of your skin to have it diagnosed. This is most commonly done under local anesthesia and involves removing the abnormality and a thin layer of the surrounding skin for examination under a microscope. After examining the sample, a Cockerell Dermatopathology dermatopathologist will provide your physician with a definitive diagnosis.
A diagnosis of melanoma will include the stage of the cancer. The stage describes to what degree, if any, the cancer has spread within the skin or to other parts of the body and is essential information for planning treatment. Your general health, age, and the subtype, location and size of the lesion will also be taken into consideration.
Common treatments for melanoma include surgical removal of the area. This is often done in the doctor’s office under local anesthesia and requires stitches for a week or two. Mohs Micrographic Surgery is the most advanced type of surgical removal, often chosen for recurring tumors and lesions in highly visible areas such as the face. Chemotherapy and radiation therapy may also be recommended. If the cancer has spread to nearby lymph nodes, the affected nodes may be surgically removed.
What is Dermatopathology?
The combination of pathology (using a microscope to identify diseases) and dermatology (diagnosing and treating diseases of the skin, nails and hair) is called dermatopathology. Dermatopathologists are highly trained physicians who examine tissue specimens under a microscope, use the medical information shared by your doctor and consult with him or her as necessary. This personal service and collaboration between your doctor and our dermatopathologists help ensure the most precise, conclusive diagnosis.
About Cockerell Dermatopathology
Cockerell Dermatopathology, located in the heart of Dallas’ medical district, was founded by Dr. Clay J. Cockerell, former president of the American Academy of Dermatology and internationally recognized dermatologist and dermatopathologist. Cockerell Dermatopathology offers diagnostic excellence and unparalleled service in the evaluation of dermatologic disorders ranging from the routine to the most difficult. To best serve referring clinicians and their patients, Cockerell Dermatopathology continues to invest in the future by implementing advanced technologies within the laboratory. These new technologies produce higher quality slides to diagnose, improves turnaround time on routine cases and allows for quicker deployment of EMR interfaces. From an academic standpoint, Cockerell Dermatopathology hosts numerous Internet-based continuing education events and has a 14-headed microscope for in-person training sessions. Cockerell Dermatopathology serves more than 800 clinicians from across Texas, the United States and abroad. With an accessible team of board-certified dermatopathologists and a highly trained support staff, Cockerell Dermatopathology’s vision is to treat every specimen as if it came from one of our own family members.
Image credit: Courtesy of the American Academy of Dermatology